




Feature Story
‘Olimbi - Mother Courage’ HIV documentary wins Geneva film festival Impact Award
16 March 2026
16 March 2026 16 March 2026At the back of the reception hall, Olimbi Hoxhaj and Karlo Mlinar are standing in disbelief. They have just won the Story Board Impact Award at the Geneva Film Festival and Forum on Human Rights (FIFDH.)
“After twenty years of leading the HIV fight in Albania, I have never won any awards in my country and here I win this big prize,” said Olimbi Hoxhaj, the protagonist of the documentary. “This is recognition for me and for all people living with HIV.”
The film focuses on Ms Hoxhaj’s plight for answers and reckoning. Her husband passed away in 2003, and no one would tell her the cause. “They kept telling me he had liver problems, but I heard a lot of whispering at the funeral and people distanced themselves,” she explained. After insisting repeatedly, she was finally told that that her husband had died of complications linked to AIDS. She herself found out she was also living with HIV as were three of her four children. Her fight thus began to obtain treatment - not available at that time in Albania - as well as get protection and raise awareness. “Without truth, there can be no dignity and with no dignity families like mine remain trapped in stigma and fear.”
“When I met Olimbi in 2019 on a flight to Tirana her story really moved me,” said filmmaker and impact producer Karlo Mlinar. At the time he was visiting his former partner who refused to start HIV treatment, being in denial about his diagnosis.
“For two years I tried to persuade him to begin treatment, relying on medical evidence, statistics and information. But it was only when he met Olimbi and heard her story that things changed,” Mr Mlinar said. Using archival footage, intimate testimony, and theatrical reconstruction, Mr Mlinar began work on his 82-minute film. He wanted to use Ms Hoxhaj’s story and her tireless work confronting stigma and institutional neglect to create a greater movement.
“’Olimbi - Mother Courage’ aims to humanize HIV via a mother’s story and educate people and get them to test, treat and prevent others from getting infected,” said Mr Mlinar.
According to Ms Hoxhaj who founded the Albanian network of people living with HIV and who is now open about her status, treatment now exists but so does stigma. “People continue to contact our association in secret and ask where they can get an HIV test without being recognized,” she said during a visit to UNAIDS Geneva headquarters. “Education is uneven so people are still diagnosed late, not because treatment is unavailable, but because fear keeps them from testing. Ending HIV will definitely require courage and compassion.”
More than 1600 people live with HIV in Albania which has a low HIV prevalence rate but new infections are on the rise, especially among men who have sex with men. In 2025, four babies were born with HIV, which Ms Hoxhaj says exemplifies the disconnect regarding testing and treatment among pregnant women.
The Balkan region has been a forgotten part of Europe in the HIV response, according to Yannis Mameletzis, consultant on HIV prevention at the World Health Organization (WHO.) “This documentary is a reminder to the public and politicians that HIV still exists and that people still die despite leaps in medical science. We cannot become complacent,” he said. Albania also remains the only country in the Balkans where there is no access to pre-exposure prophylaxis (PrEP) for key populations.
FIFDH’s Impact NGO Programme Manager Sophie Mulphin believes ‘Olimbi - Mother Courage’ can spur public health dialogue on a topic that has fallen off many people’s agenda.
“Olimbi Hoxhaj transformed personal loss into public action, helping to secure treatment for thousands. We feel Karlo’s campaign around her inspiring story has clear and achievable impact goals by reframing HIV beyond the persistent myth in the Global North of it being a disease of one community and calls for direct action - to test, treat and prevent,” she said.
Reflecting on the award, Mr Mlinar said that the (CHF 10 000) USD $12 000 cash prize was a great push for the project, which he hopes to finish in February 2027. “Information alone does not overcome fear. Stories can,” concluded Mr Milinar. Mr Mlinar and Ms Hoxhaj are still reeling from the win and their fairy tale visit to Geneva.
Region/country




Feature Story
New guidance note on decriminalizing drug use in the context of HIV
12 March 2026
12 March 2026 12 March 2026At the 69th session of the Commission on Narcotic Drugs (CND), UNAIDS, the United Nations Development Programme (UNDP) and the International Network of People who Use Drugs (INPUD), together with partners, launched a new joint guidance note titled Decriminalization of drug use in the context of HIV.
The new guidance note provides governments with practical, evidence-based recommendations on how to align drug policies with human rights standards, public health principles and the lived realities of people who use drugs.
People who use drugs are disproportionately impacted by the HIV epidemic. Globally, people who inject drugs are 14 times more at risk of contracting HIV than the general adult (15-49) population and 8% of all new HIV infections were among people who inject drugs, according to 2025 data.
More than four decades of the HIV response have shown that public health approaches are the most effective way to support people who use drugs and keep them connected to essential services, including HIV prevention, testing and treatment. Harm reduction services, including needle and syringe programmes and opioid agonist maintenance treatment, have been proven time and again to be effective in significantly reducing the risk of acquiring HIV, viral hepatitis and other blood-borne viruses. In addition, access to HIV testing and treatment can enable people living with HIV to reduce their viral load to undetectable, preventing sexual transmission of HIV.
The decriminalization of people who use drugs, combined with investments in harm reduction services, can expand access to care and enable people to seek support without fear of arrest, harassment or discrimination. However, existing punitive drug laws continue to drive millions of people who use drugs away from lifesaving HIV services, fueling stigma and discrimination and undermining progress towards global HIV targets.
“Punitive laws undermine the HIV response. Criminalization drives stigma, pushes people away from services, and weakens community-led responses. The evidence is clear,” said Eamonn Murphy, UNAIDS Regional Director for Easter Europe and Central Asia and Asia and the Pacific. “What we need now is political leadership to translate evidence into legal, policy, and financing reforms.“
The guidance note comes at a critical time for the global HIV response. As no country currently fully meets global harm reduction coverage targets, the document highlights the urgent need for legal and policy reform particularly amid financial instability in the AIDS response. This funding crunch makes it increasingly important to invest limited resources where they are most effective.
The new guidance note does not prescribe a single approach. Instead, it draws on decades of global experience and presents a range of evidence-informed approaches that countries can adapt to their national contexts including the development of clear criteria for distinguishing between drug possession for personal use and possession for supply for profit and the removal of criminal penalties for minor non-violent drug offences. It also helps policymakers work through key policy questions such as which alternative sanctions are appropriate; how not to recreate the harms of criminalization through the introduction of fines; how to ensure that referrals to treatment are voluntary and increase access to evidence‑based care; how to anticipate the potential impacts of legal and policy changes on HIV outcomes; and how to meaningfully engage communities of people who use drugs in answering these complex questions.
Communities of people who use drugs helped develop the guidelines ensuring that it responds to realities on the ground. The document outlines steps countries can take to review and reform punitive laws, expand harm reduction services, reduce stigma, and embed community leadership in national HIV responses.
“This guidance recognizes that people who use drugs must be at the centre of decisions affecting our health and rights so when lived expertise is included, HIV responses become more humane and effective,” said Anton Basenko of International Network of People who Use Drugs. The current Global AIDS Strategy for 2026-2031 calls for removing legal and policy barriers for key populations, scaling up harm reduction, and ensuring that community leadership is fully recognized and resourced. Ending AIDS as a public health threat by 2030 will not be possible without addressing criminalization and the inequalities that drive HIV vulnerability among people who use drugs.
Related




Feature Story
UNAIDS recognizes progress in West and Central Africa and urges continued commitment to end AIDS
12 March 2026
12 March 2026 12 March 2026UNAIDS has convened a Regional Dialogue on the Status of the Epidemic and the AIDS Response in West and Central Africa as part of efforts to strengthen strategic engagement for a more effective, sustainable and integrated response to HIV across the region. Addressing the meeting in her opening remarks, UNAIDS Deputy Executive Director, Angeli Achrekar highlighted the unique opportunity the year presents for global partners in the HIV response.
“This Regional Dialogue comes at a time of substantial progress towards development, for example, life expectancy has increased by 20 years in Africa since 2000. We have a unique political opportunity this year to mobilize action guided by the new 2026 – 2031 Global AIDS Strategy to end AIDS. And we have exceptional capacity for impact that can be leveraged through the power of country, regional and global partnerships,” said Ms Achrekar.
The West and Central African region has made notable progress in the AIDS response in recent years. UNAIDS data show that in 2024, 81% of people living with HIV knew their status, 76% were accessing antiretroviral therapy, and 70% had suppressed viral loads, preventing onward transmission of the virus.
Between 2010 and 2024 there was a 55% reduction in new HIV infections across the region and a 60% decline in AIDS-related deaths. However, these gains remain insufficient to meet global targets and end AIDS as a public health threat by 2030.
“The HIV epidemic is not over. It took the lives of 124,000 people in the region last year and in at least five countries in west, central and north Africa, new HIV infections continue to grow. So even as we celebrate progress, let’s remember that the job is not yet done," said Susan Kasedde, UNAIDS Regional Director, West and Central Africa.
Data from Eastern and Southern Africa show that faster progress is possible—93% of people living with HIV in the region know their HIV status, 84% are on treatment and 80% have suppressed viral loads. These results show that reaching the 2030 targets (95% of people living with HIV knowing their status, 90% receiving treatment, and 86% being virally suppressed) is achievable. The participants underscored the importance therefore of political will and engagement to accelerate progress, close gaps and end AIDS in the region.
"Behind the figures, there are still too many vulnerabilities, too many gaps in prevention, screening, and treatment services, and too many people still lack access to essential services. An even more massive remobilization of all institutional, community, and political partners and actors is necessary to meet these challenges,” said Saffiatou Thiam, Executive Direction, National AIDS Commission of Senegal.
In West and Central Africa progress is being hindered by significant inequalities which continue to persist. Disparities exist between countries and within countries, including differences across regions, districts, sexes, age groups and population groups. These inequalities limit the overall impact of interventions and threaten progress towards ending AIDS.
“To get to 2030, countries must take decisive action to protect the populations most vulnerable to HIV infection, illness and death and all those working with them. Countries must ensure that the fundamental rights of these people to life, inclusion, safety and health are not violated,” noted Magatte Mbodj, from the Alliance Nationale Contre le SIDA in Senegal.
The Regional Dialogue comes at a pivotal moment for the global HIV response. The Global AIDS Strategy 2026–2031 has recently been developed, outlining three strategic priorities:
- Sustaining the response through country-led, resilient and future-ready systems
- Putting people at the centre, ensuring equity, dignity and access to services
- Empowering communities to lead and shape the HIV response
The meeting also takes place ahead of the United Nations General Assembly High-Level Meeting on HIV/AIDS, scheduled for June 2026, which will mobilize global commitment and establish a new political declaration to guide the AIDS response for the next five years.
"In Africa, we must seize this opportunity, mobilize political leadership of the region and support and defend a strong common African position that transforms the way we think about public policy and integration, helps develop resilient systems and advances realistic, financed, achievable sub-regional targets," said Adama Bocar Soko, Deputy Resident Representative (Operations) at UNDP.
Region/country

Feature Story
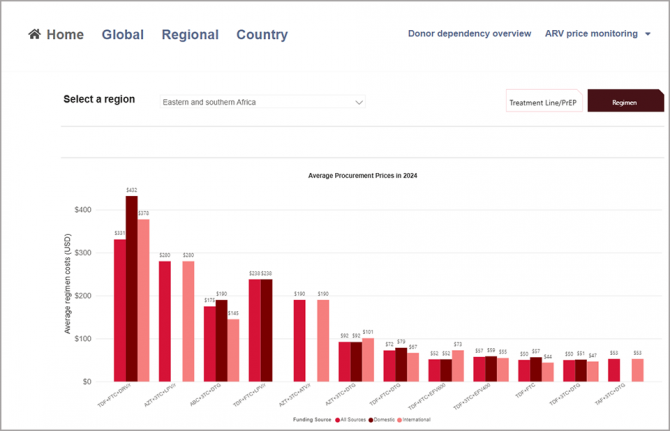
Evidence reveals cross-country price variation for the procurement of HIV treatment
05 March 2026
05 March 2026 05 March 2026UNAIDS has published its consolidated annual information on the cost of procuring antiretroviral (ARV) treatment based on data provided by countries through the UNAIDS Global AIDS Monitoring tool.
The consolidated evidence reveals that there is considerable cross-country price variation, particularly for second-line regimens where prices increase significantly with income level highlighting transition and sustainability risks in middle-income settings.
For first-line regimens, the reported data shows that international procurement channels achieve lower average prices than domestic channels, indicating opportunities for efficiency gains through competitive tendering, pooled procurement and strategic contracting.
The consolidated data, which can be accessed from the UNAIDS HIV Financial Dashboard, presents average unit prices for first- and second-line regimens, disaggregated by income group, region, country, regimen, and by domestic versus international source of procurement. This release provides strengthened financial transparency that is essential for policy dialogue and to advance global and national reforms for affordable HIV medicines.
The procurement of ARVs is a recurring, lifelong cost for every country that represent the single largest and most non-discretionary line item in their HIV budgets. As such, the stability, affordability and predictability of ARV financing are the core determinants of treatment continuity and sustained epidemic control. In an increasingly constrained fiscal environment, procurement efficiency and equitable pricing are macro-fiscal priorities and not merely technical considerations.
The new global AIDS targets include a top-line commitment on equitable pricing of medicines and therapeutics. Monitoring progress toward that target requires reliable, comparable and routinely updated price intelligence. The publication of this global reference directly supports this objective by providing a transparent basis to assess price equity across income groups and procurement modalities.
At national level, this reinforces the need for routine monitoring of ARV procurement prices as part of broader HIV financing oversight. Strengthening digital Logistics Management Information Systems (LMIS) and Procurement and Supply Management (PSM) platforms will be essential to:
- Improve real-time visibility of procurement prices and volumes
- Enhance transparency across funding sources
- Enable systematic benchmarking
- Increase efficiency and reduce avoidable cost escalation
- Carefully develop new or strengthened channels for procurement systems at national and regional levels.
“As countries navigate donor transitions, fiscal pressures and evolving treatment guidelines, systematic price monitoring must become an integral component of sustainability planning,” notes Jaime Atienza, UNAIDS Director, Sustainability Practice.
From late 2026, this global dataset will also expand to include ARVs used for pre-exposure prophylaxis (PrEP), including long-acting innovations, further strengthening its relevance for integrated HIV prevention and treatment financing.
“By consolidating, quality assuring and publishing these country-reported data as strategic financial intelligence, UNAIDS provides an essential policy tool to allow for well-planned necessary reforms, advance equitable pricing, fiscal sustainability , uninterrupted treatment access and market shaping” added Deepak Mattur, UNAIDS Senior advisor on Resource tracking.
HIV Financial Dashboard


Feature Story
Ukraine: Keeping people in care
23 February 2026
23 February 2026 23 February 2026Fifth year of war in Ukraine: deepening humanitarian needs and impact on the HIV response
In Kryvyi Rih, war is measured not only in sirens and blackouts, but in whether people can continue getting the medicines that keep them alive. The city has become a lifeline for displaced people living with or affected by HIV arriving from frontline and temporarily occupied areas—often without documents, stable housing, or a clear route back into care.
“People come to us exhausted, carrying everything they have in one bag,” says Oleksandr Shveda, a social worker at a community-run shelter operated by the charitable organization Public Health. “Some haven’t taken antiretroviral therapy for days or weeks—not because they didn’t want to, but because they lost access, lost papers and didn’t know where to turn.”
This is what Ukraine’s fifth year of war looks like for the HIV response: care delivered through delays, danger and uncertainty, often to people who are least visible and most excluded.
People living with HIV and other groups vulnerable to HIV can be overlooked by mainstream humanitarian and social protection programmes. Many people from key populations remain marginalized and fall outside the “typical” categories reached by humanitarian assistance and social protection programmes, even though they face some of the highest health and protection risks. In wartime, when systems are overstretched and priorities narrow, these communities can fall even further out of reach.
“They often try to stay invisible,” explains social worker Olena Maligina. “But HIV doesn’t wait, and neither does Tuberculosis. Keeping someone in care is not just about medicine—it’s about safety and trust.”
Continuity of HIV care is not only a matter of individual survival; it is a public health necessity. Maintaining treatment, counselling and referral pathways helps prevent interruption, reduces severe illness, limits onward transmission, and supports reintegration upon release.
However, with limited staff capacity, reliance on volunteers, and close coordination with national partners, the team at the Public Health organization says it is becoming harder to reach the people most at risk—especially medically fragile people living with HIV, including palliative and bedridden patients. “We are doing everything we can,” Mr Shveda adds, “because for some people, this support is the only bridge to life and dignity.”
Across the country, the humanitarian crisis continues to deepen, with profound consequences for access to essential services, including health care. In frontline areas, intensified hostilities have left health facilities damaged or non-functional, created severe staff shortages, and made it unsafe for ambulances to reach remote or heavily affected areas. For HIV services, the energy crisis has become an ongoing barrier to continuity. Power outages disrupt clinic operations, laboratories, health information systems, telecommunications and transport—making it harder for health workers to deliver services and for people living with HIV to access care and remain on treatment.
The combined pressures of protracted conflict, displacement, poverty, and infrastructure damage are eroding coping capacities and increasing the risk of HIV treatment interruption. In this environment, community-led and community-based responses remain central to maintaining reach, trust and continuity, especially for people facing insecurity, displacement and social vulnerability. Yet these organizations are under growing strain: staff capacity is shrinking, burnout risks are rising, and operational constraints make every visit, delivery and follow-up more difficult.
The Government of Ukraine, through the Ministry of Health and the Ukraine Public Health Center, continues to lead the national response in close partnership with community organizations to sustain services under wartime conditions. Support from international partners and donors—especially the United States Government, the Global Fund to Fight AIDS, Tuberculosis and Malaria, Expertise France, the Government of the Netherlands, and other bilateral and multilateral partners—has been critical to maintaining essential HIV prevention, testing, treatment and care.
“Ukraine’s resilience is visible in the remarkable courage of its people—and in the determination of health-care workers and community organizations who keep services going when conditions make it feel impossible,” says Eamonn Murphy, UNAIDS Regional Director for Easter Europe and Central Asia and Asia and the Pacific. “They keep services open, reach people on the move, and ensure no one is left without care. Their work is built on trust, and in this war, that trust can be lifesaving. We must continue supporting community-led services so people can stay on treatment safely and with dignity.”
In 2026, the AIDS response will remain heavily dependent on external support, underscoring the need for strategic, predictable funding to sustain essential services while also beginning, where it is feasible, to plan a gradual transition towards nationally owned systems and community-led structures.
The message from Kryvyi Rih is clear: continuity of care is not automatic in a war—it is built, protected and must be sustained.
Region/country
Related
 Women, HIV, and war: a triple burden
Women, HIV, and war: a triple burden

12 September 2025
 Displacement and HIV: doubly vulnerable in Ukraine
Displacement and HIV: doubly vulnerable in Ukraine

11 August 2025




Feature Story
Benin adopts positive new law on HIV prevention, care and elimination of stigma and discrimination
20 February 2026
20 February 2026 20 February 2026UNAIDS welcomes the passing into law by the President of Benin Patrice Talon of Law 2026-02 on 9 February 2026. The law focuses on HIV prevention and management of care and will accelerate progress towards ending AIDS in the Republic of Benin.
The new law is the culmination of a process first initiated in 2013 and which resumed in 2020 under the leadership of the Health Program for the Fight against AIDS (PSLS). This revision was made due to the significant limitations of the 2006 law, namely that it was based on a punitive, coercive and stigmatizing approach.
The previous law was incompatible with human rights standards, allowed for numerous violations of confidentiality, criminalized HIV-related behaviors and reinforced the marginalization of key populations. The law was out of step with good public health practices which should be based on prevention, inclusion and respect for human rights.
The 2026 law is now aligned with international human rights standards and more specifically reaffirms the right to non-stigma and non-discrimination. It enhances privacy and data protection, ensures access to HIV care and prevention and services and recognizes key populations including sex workers, men who have sex with men, people who inject drugs, transgender people, migrants and prisoners among others. It improves prisoners’ rights significantly and reduces criminal provisions against people living with HIV by recognizing the strictly voluntary nature of disclosing HIV status.
“The journey to validating Benin’s HIV Law was powered by strong country leadership, exceptional UNAIDS–UNDP collaboration, unwavering support from the UN Regional Coordinator, close technical follow-up with the Ministry of Health, catalytic funding from UNAIDS, UNDP and Expertise France, and close involvement of parliamentarians — turning evidence into political will and political will into transformative legislation’’ said Yayé Diallo, outgoing UNAIDS Country Director for Togo and Benin.
The progress is the result of coordinated advocacy and collaborative partnership actions at all levels involving the UNAIDS Executive Director Winnie Byanyima, who made it a priority of her visit to Benin in September 2024.
UNAIDS Regional Office, the global HIV Legal Network and UNDP provided technical support. The Global Fund and Expertise France provided financial support and the combination of the efforts of various stakeholders at the local level, namely the PSLS, the CNLS-TP(Conseil National de Lutte contre le VIH/Sida, la Tuberculose, le Paludisme, les Hépatites, les Infections Sexuellement Transmissibles et les Épidémie), the parliament and its institutions (IPaB - Institut Parlementaire du Bénin), the caucus of women parliamentarians and parliamentary committees), civil society organizations including networks of people living with HIV and key populations. With this new law and rigorous monitoring of its application, Benin is resolutely committed to its march towards the ending AIDS by 2030.
"UNAIDS, the UN Country Team, and partners including Expertise France applaud Benin’s political resolve and its new, pioneering HIV legislation. By centering the law on vulnerable groups and youth who account for 35% of new infections, Benin is taking a giant leap towards universal access to HIV treatment and the ultimate goal of ending AIDS as a public health threat by 2030." said Christian Mouala, Representative and Director of the UNAIDS Multi-Country Office for Côte d’Ivoire, Togo, and Benin.
Region/country
Related


Feature Story
Strengthening partnerships to sustain the HIV response in Eastern Europe and Central Asia
12 February 2026
12 February 2026 12 February 2026“We’re closely watching developments in both infection rates and funding in Eastern Europe and Central Asia. The challenges are great,” said Anne von Fallois, CEO of Deutsche AIDS-Stiftung (DAS), during a meeting with Eamonn Murphy, UNAIDS Regional Director, in Bonn. “We’re united on the importance of the region—especially Ukraine.”
This is a critical moment for the AIDS response in Eastern Europe and Central Asia (EECA). As global attention shifts to new crises, there is growing concern that the region—where both new HIV infections and AIDS-related deaths are still rising—could be left behind.
Since 2010, AIDS-related deaths in EECA have increased by 34%. Only about half of people living with HIV are on treatment, and viral suppression—at just 42%—is the lowest globally. More than half of new HIV diagnoses occur late, when risks of transmission and mortality are significantly higher.
War, displacement, economic hardship, and migration may be contributing to a more challenging HIV response, with potential implications beyond national borders, including the European Union. While the full impact is still emerging, these pressures could place additional demands on health systems and underscore the importance of sustained, coordinated action.
Access to services remains fragile in all countries of the region. While antiretroviral therapy is officially free in most countries, too many people are still unable to access it. Prevention coverage is even lower: opioid agonist maintenance therapy reaches only a fraction of those who need it, and pre-exposure prophylaxis remains limited. Key populations account for most new infections, yet continue to face stigma, discrimination, and legal barriers rooted in outdated policies.
“We know what works: community-led services are essential to reach people who are otherwise excluded, and partnership with communities is vital in these challenging times,” said Eamonn Murphy. “With continued UNAIDS engagement in the region, sustained, coordinated investment—alongside government commitment and community engagement—is essential to protect progress and prevent further loss of life.”
Through its partnership with UNAIDS, Deutsche AIDS-Stiftung supports HIV work in Germany and internationally, advancing stigma reduction, prevention, social support, and assistance for vulnerable groups.
As funding uncertainties grow, partners stressed the need to strengthen joint resource mobilization and encourage more active engagement from the European Union. Emergency measures can only go so far. The investments required are modest, but the stakes—for the region and for Europe as a whole—could not be higher.


Feature Story
‘I never lacked anything—except answers’ - a young man’s journey of being born with a disease he did not understand
19 January 2026
19 January 2026 19 January 2026For 24-year-old Rakhants’a Lehloibi, growing up in the rural village of Maphutseng, in Lesotho, meant navigating life with a secret he didn’t fully understand. Born with HIV, he spent his earliest years believing the antiretroviral (ARV) treatment he took daily was simply to stop frequent nosebleeds—a story his grandmother told to shield him from the stigma surrounding HIV.
“Life was tough, but my grandmother gave me all the love in the world,” he recalled. “I never felt like I lacked anything—except answers.”
Rakhants’a’s mother died when he was very young, leaving his grandmother to raise him. In 2007, when he was just 4 years old, he became severely ill. Traditional healers were consulted, but their remedies failed. It was only when he was taken to a local clinic that he was tested and diagnosed with HIV.
“Back then, I didn’t even know what HIV was,” he said. “My grandmother told me the pills I was taking were to stop nosebleeds. I believed her.”
In Lesotho—as in much of sub-Saharan Africa—stigma against people living with HIV remains widespread. Many conceal their status to avoid rejection by family and community.
“For years, I took pills but I didn’t understand why. I missed school for clinic visits. I watched my grandmother struggle just to make sure I got my medication,” Rakhants’a said. Eventually, doubting the need for treatment since his nosebleeds stopped, he began skipping doses. “I didn’t know I was putting my life at risk.”
The stigma he faced only deepened his struggle. “Kids at school whispered that I had AIDS. I felt isolated, ashamed and angry. I even thought about running away just to escape the pain. But I kept going. I passed my exams and later moved to the country’s capital Maseru to live with my sister and attend high school.”
UNAIDS country Director for Lesotho, Pepukai Chikukwa, agrees that "Though HIV stigma has reduced over the years, it is still a critical barrier to the AIDS epidemic, obstructing access to life-saving HIV prevention and treatment." Ms Chikukwa adds that it pushes people away from care and increases their risk of infection. Ms Chikukwa noted that “Addressing HIV-related stigma and discrimination requires a coordinated, multi-level, and multi-setting approach involving individuals, communities, organizations and policymakers.”
It was in Maseru that Rakhants’a’s life began to change. At Baylor Clinic, he finally learned the truth about his diagnosis and joined the Teen Club, a support network for young people living with HIV.
“For the first time, I met others like me. I realized I had been born with HIV, passed on from my late mother. That was a turning point.”
Still, the journey was not easy. Poor adherence to HIV treatment meant that Rakhants’a’s viral load was dangerously high. One health worker bluntly told him he was “as good as dead.” Placed on second-line treatment—five pills a day instead of one—he felt overwhelmed.
“At first, it was hard. But instead of giving up, I prayed every day and asked my mother to watch over me. Slowly, things changed. I gained strength, I took my medication properly, and within three months, my viral load was suppressed.”
Today, Rakhants’a uses his voice to fight stigma and inspire others. Through social media and community platforms, he spreads a message of hope and resilience.
“Being HIV positive doesn’t mean your life is over,” he said. “With proper treatment and support, we can live full, healthy lives.”
According to UNAIDS, there are 260,000 people living with HIV in Lesotho and 3200 people became newly infected with HIV in 2024. There were 6,400 children aged between 0 to 14 years, living with HIV. Nonetheless, 97% of people living with HIV know their status, of those, 97% are receiving HIV treatment and 99% of those are virally suppressed. In 2023, 11.3% of women and 18.5% of men aged 15 – 49 years old reported discriminatory attitudes toward people living with HIV.
Region/country
Related


Feature Story
UN Deputy Secretary-General reaffirms commitment to a responsible UNAIDS transition and UN commitment to the AIDS response at Board meeting
22 December 2025
22 December 2025 22 December 2025The United Nations Deputy Secretary-General, Amina Mohammed, joined the 57th meeting of the UNAIDS Programme Coordinating Board (PCB) in Brasilia, bringing a clear message: the UN will stand with governments and communities until AIDS is ended as a public health threat.
In her remarks to the Board, the Deputy Secretary-General commended the inclusive and constructive nature of the deliberations and reaffirmed that the ongoing UN80 reform process will strengthen – not diminish – the global AIDS response. She stressed that reform must be deliberate and protect what works. “There is a sense of urgency, but let me underscore here, we are not in a hurry to fail... We must achieve common ground around all the concerns that the PCB and civil society have aired over the last few weeks in particular,” she said.
Ms. Mohammed warned of growing financial pressures on countries and donors, highlighting the strain on domestic resources in low- and middle-income countries, driven by debt and the cost of debt servicing. “Governments, even if they wanted to prioritize HIV and AIDS as a budget spend, quite frankly are taking away from education, taking away from health, because they cannot meet that [cost],” she said. “Part of what we have to do today with this strategy and with the transitions that we offer in UN80 – and UNAIDS is one of them – is how to convince the international community to come back.”
The UN80 initiative aims to make the UN development system more coherent, integrated, and fit for purpose in a rapidly changing world. For UNAIDS, this means a two-phase transition that preserves its core functions and highest-value contributions to the global AIDS response – leadership and advocacy, convening and coordination, accountability and data, and community engagement.
During its meeting, the PCB adopted landmark decisions that will shape the next phase of the HIV response:
- Global AIDS Strategy 2026–2031: A bold, evidence-informed roadmap grounded in human rights, gender equality, and community leadership. The strategy will guide preparations for the 2026 UN General Assembly High-Level Meeting on AIDS and negotiations for the political declaration.
- UNAIDS and UN80 transition: The Board reaffirmed its commitment to a responsible, inclusive transition of the UNAIDS Joint Programme within the wider UN development system. A PCB Working Group will be established in early 2026 to ensure the process is orderly, transparent, and safeguards UNAIDS’ core functions.
“I have seen many across the agencies that I chair in the UN Sustainable Development Group … This is a really good one. Why? Because it has so much clarity, it has so much of a division of labour, but I think that in this particular case, what has helped it is this nature of inclusion that you have had, and demonstrated, in the PCB, with civil society having such a strong voice,” said Ms Mohammed.
The PCB meeting also featured a one-day thematic discussion on long-acting antiretrovirals, highlighting their potential to transform HIV prevention and treatment. With political will, financing, and partnerships, these innovations can dramatically reduce new infections and accelerate progress toward ending AIDS.
“Ending AIDS remains achievable,” she concluded. “But only if resources match our ambition.”




Feature Story
Multisectoral resilience to funding cuts in Guatemala
22 December 2025
22 December 2025 22 December 2025This story first appeared in the recently released World AIDS Day report 2025.
In 2025, cuts in international support for the HIV response in Guatemala and a reduced HIV allocation from the Global Fund caused immediate challenges for the HIV response. Some services were curtailed or discontinued altogether in clinics affected by the cuts, and remaining service providers struggled to absorb clients who had lost their service access. Furthermore, a substantial portion of the personnel at HIV comprehensive care units and community outreach workers that help facilitate and maintain access to services for people from key populations were also affected as their work had long been funded by external donors.
In response to these cuts in external funding, the Ministry of Health stepped in to ensure continuity of care by covering the salaries of 81 staff members, thereby sustaining the operation of numerous comprehensive care units and guaranteeing service delivery to thousands to clients across the country. This intervention was critical to maintain access to lifesaving HIV treatment and preserve the integrity of the national HIV response.
The Government also intervened to fill the gap when a key implementer and PrEP provider lost its financing. In 2025, Guatemala moved to quantify PrEP needs, develop targets for scale-up and launch access to PrEP in three departments. However, gaps persist with respect to HIV prevention programmes for people from key populations.
Community-led responses have also stepped into the breach created by the loss of international assistance. Colectivo Amigos contra el Sida (CAS), an organization focused on HIV prevention among gay men and other men who have sex with men and transgender women, moved to assume responsibility for supporting PrEP delivery to clients of a large PrEP programme that lost its funding. CAS collects voluntary donations for services from clients who can afford to pay, which helps to co-finance operational costs that are no longer covered by international donors.
Community-led responses play a critical role in the efforts to end AIDS as a public health threat. For that reason, Guatemala, with the support of UNAIDS, is working to ensure communities have access to financial and technical support. UNAIDS is collaborating with the Global Fund to help build the knowledge and capacity of civil society organizations to lobby more effectively for greater domestic resources.
Planning for the sustainability of the HIV responses is an urgent priority for many countries including Guatemala. Now that the Global Fund is set to phase out its support given Guatemala’s status as an upper-middle-income country, UNAIDS is collaborating with the Ministry of Health and the national AIDS programme to roll out the UNAIDS Rapid AIDS Financing Tool, aimed at facilitating decision-making and actions to effectively respond to the AIDS epidemic amidst a resource-limited environment.




















